Despite efforts to improve price transparency, 43 states received an "F" grade according to the Health Care Incentives Improvement Institute (HCI3 ) – Catalyst for Payment Reform (CPR) Report Card on State Price Transparency Laws.
 In nearly every industry, we expect to know how much we will pay for goods and services.As this report confirms, the answer of "how much does it cost?" in healthcare is still blurry at best.
In nearly every industry, we expect to know how much we will pay for goods and services.As this report confirms, the answer of "how much does it cost?" in healthcare is still blurry at best.
According to the report, "we find that too many states still fall far short of requiring and implementing thorough, useable transparency resources. Dozens of states have laws that refer to price transparency, but provide little to help consumers shop for and choose care, and ofer little potential to move the health care delivery system toward quality and afordability."
Here is how each state was scored:
- A 150-point scale was used, with 100 points available based on a state's price transparency laws and regulations.
- If pricing information was only available to consumers from providers, the state could earn 50 points based upon a number of factors, including the pricing information available and how the pricing information is disclosed.
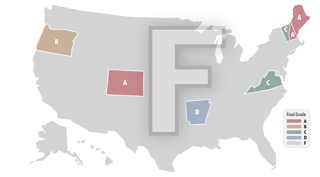
The seven states to receive a passing grade:
- Colorado ("A")
- Maine ("A")
- New Hampshire ("A")
- Oregon ("B")
- Virginia ("C")
- Arkansas ("D")
The full report card is available here.
As states continue to get scrutinized by reports like these, it's likely that we will see movement in price transparency legislation. Another 10 states -- Alabama, Georgia, Hawaii, Michigan, Missouri, New Jersey, Oklahoma, Pennsylvania, Texas, West Virginia -- have prepared bills directing hospitals and clinicians to consumers pricing information prior to care and are recognized in the report as moving in the right direction.
As legislation gains momentum, more and more hospitals will look toward providing accurate, up-front patient estimates.


